This article explains how biomarker analysis methods are used in both clinical medicine and functional health settings. It clarifies what biomarkers measure, how the same laboratory tests are interpreted differently for diagnosis versus prevention, and why accuracy, limitations, and professional oversight are essential for responsible use. Key points covered in this guide: What biomarkers measure …
This article explains how biomarker analysis methods are used in both clinical medicine and functional health settings. It clarifies what biomarkers measure, how the same laboratory tests are interpreted differently for diagnosis versus prevention, and why accuracy, limitations, and professional oversight are essential for responsible use.
Key points covered in this guide:
- What biomarkers measure and why they matter
- Differences between clinical and functional interpretation
- Accuracy, limitations, and the need for clinical oversight
Biomarkers play a central role in modern healthcare by providing measurable insights into physiological processes, disease risk, and overall health status. As laboratory science has advanced, biomarker analysis methods have expanded beyond traditional diagnostic testing to include broader functional assessments used in preventive and personalised care. Understanding how these methods differ, and how they are applied in clinical versus functional contexts, is essential for interpreting results accurately and using them responsibly.
What Are Biomarkers?
Biomarkers, or biological markers, are objectively measurable indicators of biological processes occurring within the body. They can reflect normal physiological function, pathological changes, or responses to therapeutic interventions. Biomarkers are typically measured in biological samples such as blood, urine, saliva, or tissue, and are interpreted within established scientific and clinical frameworks.
In conventional medicine, biomarkers are most commonly used to support diagnosis, monitor disease progression, or evaluate treatment response. In functional and preventive settings, biomarkers may also be used to assess trends, identify early deviations from optimal ranges, and inform personalised health strategies.
Categories of Biomarkers
Biomarkers are often grouped based on what they measure and how they are used.
Diagnostic Biomarkers
Diagnostic biomarkers are used to confirm or rule out the presence of disease. Examples include fasting blood glucose for diabetes diagnosis or troponin levels in the assessment of acute cardiac events. These biomarkers are interpreted against validated clinical thresholds.
Prognostic Biomarkers
Prognostic biomarkers provide information about the likely course of a disease, independent of treatment. They help estimate risk, progression, or long-term outcomes.
Predictive Biomarkers
Predictive biomarkers indicate the likelihood of response to a particular therapy. These are commonly used in oncology and pharmacogenomics.
Monitoring Biomarkers
Monitoring biomarkers are measured repeatedly to track disease activity or treatment effectiveness over time, such as inflammatory markers or lipid profiles.
Risk and Susceptibility Biomarkers
These biomarkers identify increased likelihood of developing a condition, often before symptoms appear. Genetic markers frequently fall into this category.
Common Biomarker Analysis Methods
Blood-Based Biomarker Testing
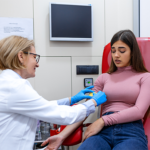
Blood analysis remains the most widely used biomarker testing method. It allows measurement of hormones, enzymes, metabolites, inflammatory markers, lipids, vitamins, minerals, and immune indicators. Blood biomarkers are central to both diagnostic medicine and functional health assessment due to their reliability and standardisation.
Urine-Based Biomarker Testing
Urine biomarkers are used to assess kidney function, metabolic by-products, hormone metabolites, and exposure to certain substances. They are particularly useful for evaluating excretion patterns and metabolic balance.
Saliva-Based Biomarker Testing
Saliva testing is used for specific hormone measurements, such as cortisol, particularly when assessing diurnal patterns. While less invasive, saliva testing has more limited applications and requires careful interpretation.
Genetic and Genomic Biomarker Testing
Genetic biomarkers identify inherited variations that may influence disease risk, metabolism, or drug response. These markers remain stable throughout life and are used primarily for risk assessment and personalised care planning rather than diagnosis.
Clinical Biomarker Analysis. Purpose and Methodology
Clinical biomarker analysis is grounded in evidence-based medicine and regulatory standards. Tests are validated through large population studies, and results are interpreted against established reference ranges.
Key Characteristics of Clinical Biomarker Analysis
- Used to diagnose, monitor, or manage disease
- Based on validated thresholds and guidelines
- Interpreted in conjunction with symptoms, imaging, and clinical examination
- Governed by regulatory and professional standards
Clinical biomarkers are designed to answer specific medical questions, such as whether a disease is present or whether treatment is effective.
Functional Biomarker Analysis. Purpose and Methodology
Functional biomarker analysis focuses on understanding physiological trends, metabolic balance, and early deviations from optimal function. Rather than asking whether disease is present, functional analysis explores how well systems are operating and whether patterns suggest emerging risk.
Key Characteristics of Functional Biomarker Analysis
- Emphasises trends and patterns rather than single thresholds
- May use optimal or functional ranges alongside clinical reference ranges
- Often applied in preventive and wellness contexts
- Requires careful clinical interpretation to avoid overdiagnosis
Functional analysis does not replace clinical diagnostics. Instead, it provides additional context that may support early intervention strategies.
Healthspan Focused Biomarker Testing. Going Beyond Traditional Blood Tests
In healthspan and prevention focused care, biomarker analysis extends beyond standard diagnostic panels to identify early risk patterns that may not yet be captured by conventional testing. These biomarkers are not used to diagnose disease, but to assess physiological stress, emerging risk, and long term health trajectories.
For cardiovascular risk assessment, apolipoprotein B and lipoprotein(a) are increasingly used alongside traditional lipid profiles. Apolipoprotein B reflects the total number of atherogenic lipoprotein particles, offering a more precise measure of cardiovascular risk than cholesterol levels alone. Lipoprotein(a) provides insight into genetically driven cardiovascular risk that is not detected through standard lipid testing and is strongly associated with heart attack risk.
In metabolic health assessment, both fasting insulin and fasting glucose are measured together to evaluate insulin resistance. Insulin resistance can develop silently for years before blood glucose levels rise into the diabetic range, making early detection particularly important in preventive health strategies.
To assess systemic inflammation, high sensitivity C reactive protein (hs CRP) is used to measure background, low grade inflammation that is not captured by traditional inflammatory markers. Chronic low grade inflammation is recognised as a key factor that accelerates multiple disease processes, including cardiovascular disease, neurodegenerative conditions such as dementia, and cancer.
When interpreted within appropriate clinical context, these biomarkers provide deeper insight into long term health risk and physiological resilience, supporting earlier and more personalised preventive strategies.
Key Differences Between Clinical and Functional Approaches
| Aspect | Clinical Approach | Functional Approach |
| Primary purpose | Diagnosis and disease management | Prevention and optimisation |
| Reference ranges | Population-based clinical ranges | Functional or optimal ranges |
| Interpretation | Binary or threshold-based | Trend and pattern-based |
| Regulatory role | Central to medical decision-making | Supportive and adjunctive |
| Risk tolerance | Low | Requires careful interpretation |
Both approaches rely on the same laboratory measurements. The distinction lies in how results are interpreted and applied.
Accuracy and Reliability of Biomarker Testing
Accuracy in biomarker analysis depends on multiple factors, including sample handling, laboratory quality, biological variability, and clinical context. No biomarker provides absolute certainty in isolation. Interpretation must consider age, sex, lifestyle, medications, and underlying conditions.
Repeated measurements and longitudinal tracking often provide more meaningful insights than single test results, particularly in functional assessments.
Clinical Oversight and Interpretation
Biomarker analysis requires professional oversight. Misinterpretation can lead to unnecessary anxiety, inappropriate supplementation, or delayed medical care. Clinical judgement is essential in determining which biomarkers are relevant, how results should be interpreted, and what actions, if any, are appropriate.
Biomarker Analysis at Elite Vita
Biomarker analysis services at Elite Vita involve structured testing of blood and other biological markers to provide insight into cardiovascular health, metabolic function, inflammation, immune activity, and genetic risk factors. These assessments are used to inform personalised health planning through a precision medicine approach, integrating clinical interpretation with individual health context.
Who Can Benefit From Biomarker Analysis?
Biomarker analysis may be valuable for:
- Individuals seeking preventive health insights
- Those managing chronic conditions under medical supervision
- People interested in understanding metabolic or inflammatory trends
- Individuals exploring personalised health strategies
It is not a substitute for medical diagnosis or treatment, and results must always be interpreted within appropriate clinical frameworks.
Summary
Biomarker analysis methods form the foundation of both modern clinical medicine and emerging personalised health approaches. Clinical and functional frameworks differ primarily in interpretation rather than measurement. When applied responsibly, biomarker testing can provide meaningful insight into health status, risk, and physiological function without replacing clinical diagnosis or care.
FAQs
What are the most common biomarker analysis methods?
Blood, urine, saliva, and genetic testing are the most commonly used biomarker analysis methods.
Are biomarker tests used for diagnosis?
Yes, many biomarkers are used diagnostically, while others are applied for monitoring and risk assessment.
How accurate is biomarker analysis?
Accuracy depends on laboratory standards, biological variability, and appropriate clinical interpretation.
What is the difference between clinical and functional biomarker analysis?
Clinical analysis focuses on diagnosis and disease management, while functional analysis evaluates trends and physiological balance.
Who can benefit from biomarker analysis?
Individuals seeking preventive insights, personalised health planning, or monitored care under professional supervision may benefit.