This article explains how PCOS is diagnosed using clinical criteria supported by hormone testing and imaging rather than a single lab result. It clarifies what PCOS blood markers show, how results are interpreted in context, and why structured medical evaluation is required for accurate diagnosis. It also outlines how integrated hormone and DNA based assessment …
This article explains how PCOS is diagnosed using clinical criteria supported by hormone testing and imaging rather than a single lab result. It clarifies what PCOS blood markers show, how results are interpreted in context, and why structured medical evaluation is required for accurate diagnosis. It also outlines how integrated hormone and DNA based assessment can support personalised health planning.
Key points covered in this guide:
- How PCOS diagnosis is made using combined clinical criteria
- What PCOS blood tests measure and how they are interpreted
- Why lab results alone are not sufficient for confirmation
Many people begin their hormone health journey by searching for a pcos test and expect a single report to give a clear answer. In clinical practice, diagnosis is more structured and more careful than that. Polycystic Ovary Syndrome is identified through a combination of symptom patterns, hormone measurements, imaging findings, and exclusion of other endocrine conditions that can look similar at first glance.
Understanding how testing actually works helps reduce confusion and prevents over reliance on one lab value. This guide explains how PCOS is diagnosed clinically, what blood analysis contributes, how results are interpreted, and how integrated wellness assessment at Elite Vita supports individuals with structured testing and DNA based biological insight.
Why There Is No Single Definitive Test
PCOS is a clinical syndrome, not a single marker disease. That means doctors do not diagnose it from one number or one scan. Instead, they use recognised diagnostic criteria that look at patterns across menstrual function, androgen activity, and ovarian structure.
Most clinical frameworks require at least two of the following three features. Irregular or absent ovulation. Signs of androgen excess. Polycystic ovarian morphology on ultrasound. Other medical causes must be ruled out before confirmation.
Because of this, testing is layered. Lab work supports the diagnosis, but it does not replace clinical judgement. This is an important expectation to set early.
What Blood Testing Adds To The Diagnostic Picture
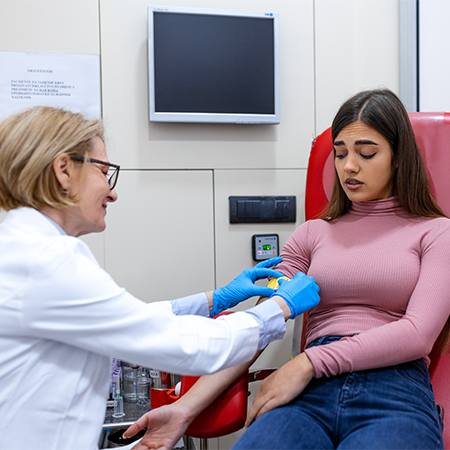
Hormone analysis plays a supporting role in evaluation. A pcos blood test helps clinicians understand endocrine signalling, androgen exposure, and metabolic status. It also helps rule out thyroid and prolactin disorders that can produce similar menstrual changes.
Blood markers are interpreted alongside symptoms and cycle history. They are not read in isolation. Timing within the menstrual cycle, medication use, and laboratory reference ranges all influence how results are understood.
A common online question is can pcos be detected in blood test results alone. The precise clinical answer is that hormone patterns can strongly support suspicion, but laboratory findings by themselves are not sufficient for confirmation.
Hormones Commonly Measured In Evaluation
A structured pcos lab test panel usually includes reproductive and regulatory hormones selected based on symptoms. The aim is to understand androgen levels, ovulatory signalling, and upstream endocrine control.
Androgen measurements are often central to the panel. These may include testosterone fractions and adrenal androgens. Elevated values can align with clinical features such as persistent acne, excess facial or body hair, or scalp hair thinning.
Pituitary signalling hormones are also reviewed to understand ovarian communication patterns. These values help clinicians judge whether ovulation is occurring regularly or not. Thyroid markers and prolactin are commonly included because disturbances in these systems can disrupt cycles and must be excluded before diagnosis is made.
Some hormone values vary across the cycle, so clinicians interpret them in timing context rather than as fixed numbers.
Metabolic Markers And Why They Are Reviewed
PCOS is not only about reproductive hormones. It is also associated with metabolic regulation, particularly insulin response. For that reason, metabolic markers are often reviewed as part of the broader assessment.
Glucose regulation markers and lipid patterns are reviewed to understand underlying metabolic function and longer term risk. Measures such as fasting glucose and insulin help identify early insulin resistance, which can be present years before overt metabolic disease develops. Lipid markers provide additional context around cardiometabolic risk and help inform personalised management once a clinical diagnosis is established. These findings guide lifestyle and nutritional planning once a clinical conclusion is reached.
Metabolic values do not determine whether the syndrome is present. They help shape personalised management after diagnosis.
The Role Of Ultrasound Imaging
Pelvic ultrasound is often used to examine ovarian structure and follicle distribution. Some individuals show a higher number of small follicles and increased ovarian volume. This pattern is called polycystic ovarian morphology.
Imaging must be interpreted carefully. Similar patterns can appear in people without the syndrome, especially in younger age groups. Some affected individuals may not show classic morphology at all. Ultrasound therefore supports the clinical picture but does not define it alone.
This combined approach explains why how to test for pcos is not answered by one scan or one lab report. It is a coordinated clinical pathway.
How Clinical Testing Usually Proceeds
When patients ask how to get tested for pcos, the correct pathway is structured medical evaluation. The process begins with detailed history taking. Menstrual timing, symptom changes, skin and hair patterns, weight shifts, and reproductive history are reviewed carefully.
A focused examination may follow. Laboratory testing is then selected according to the symptom pattern. Imaging is added when appropriate. Additional endocrine causes are excluded through targeted testing.
This stepwise approach improves accuracy and reduces both over diagnosis and missed diagnosis. Self ordered isolated hormone panels without clinical interpretation often create more confusion than clarity.
Symptom Patterns That Commonly Trigger Testing
Testing is usually prompted by ongoing symptom clusters rather than one isolated complaint. Menstrual irregularity is one of the most common triggers. This includes infrequent cycles, long gaps between periods, or absent periods.
Androgen related skin and hair changes are another frequent reason for investigation. These include persistent adult acne, increased facial or body hair, and scalp hair thinning. Difficulty conceiving can also lead to evaluation.
Symptom intensity varies widely. Some individuals show mild visible symptoms with clear biochemical shifts. Others show strong symptoms with only modest laboratory changes. Clinical interpretation weighs both elements together.
Limits Of Lab Values Alone
Hormone results must always be read in context. Values shift across the menstrual cycle and across life stages. Reference ranges differ between laboratories. Medicines such as hormonal contraception can significantly alter readings.
A single normal result does not always exclude the condition. A single abnormal result does not confirm it. Repeat testing is sometimes recommended when results are borderline or when timing was uncertain.
For this reason, pcos diagnosis remains clinically anchored. Laboratory data supports the decision but does not replace medical judgement.
Integrated Hormone And DNA Based Insight At Elite Vita
At Elite Vita, hormone and metabolic assessments are approached through medically supervised and evidence informed evaluation. Laboratory testing is coordinated with symptom history and clinical review so that results are interpreted responsibly rather than in isolation.
Where appropriate, broader biological context may also be included through advanced genetic analysis. Our DNA testing service provides personalised insight into metabolism, nutrient handling, inflammation response, and lifestyle sensitivity patterns. This form of analysis is not used to diagnose hormonal syndromes. It is used to support more tailored wellness and prevention strategies alongside clinical findings.
This integrated model allows laboratory data, clinical patterns, and genetic context to be considered together in a structured way.
Why Personal Context Changes Interpretation
Hormonal health does not exist separately from lifestyle, sleep quality, nutrition, stress load, and genetic background. Two people with similar lab values can experience very different symptom patterns and outcomes.
That is why responsible clinical interpretation focuses on the whole picture. Hormone levels, metabolic markers, symptom history, and biological tendencies together produce a more useful planning framework than any single metric.
Personal context improves decision quality and expectation setting.
When Professional Evaluation Is Advisable
Persistent menstrual irregularity, androgen related symptoms, or unexplained fertility difficulty should be evaluated clinically rather than self diagnosed. Early structured assessment supports clearer answers and appropriate monitoring.
Professional evaluation also helps distinguish this syndrome from other endocrine disorders that require different management approaches. Structured review reduces the risk of misinterpretation from fragmented online information.
For personalised evaluation and medically guided testing support, you can contact our clinical team here:
FAQs
What tests are done to confirm PCOS?
Confirmation uses combined clinical criteria supported by hormone analysis, menstrual history, symptom review, and often ultrasound imaging, with other endocrine causes excluded.
How do I confirm if I have PCOS?
Confirmation requires medical evaluation using accepted diagnostic criteria and integrated interpretation of symptoms, laboratory findings, and imaging.
What tests are needed to diagnose PCOS?
Hormone panels, metabolic markers, and pelvic imaging are commonly used alongside clinical assessment.
What are the warning signs of PCOS?
Irregular cycles, androgen related skin or hair changes, and fertility difficulty are common warning patterns.
What are the 5 symptoms of PCOS?
Frequently reported features include cycle irregularity, acne, excess hair growth, scalp hair thinning, and ovulatory difficulty.
What’s the biggest symptom of PCOS?
There is no single dominant feature. Menstrual irregularity is one of the most frequently reported signs.
How do I know I am PCOS?
Symptoms alone cannot confirm it. A structured clinical evaluation is required.
What is the first stage of PCOS?
There is no formal staging system. Diagnosis is criteria based rather than stage based.
What is a corpus luteum cyst PCOS?
A corpus luteum cyst is a functional ovulatory cyst and is different from this syndrome.
What is stage 3 of PCOS?
There is no recognised stage classification in standard diagnostic frameworks.
What are the red flags of PCOS?
Ongoing cycle disruption combined with androgen related symptoms and fertility challenges are considered strong clinical flags.